 Hi, my name is Kemporn “Pom” Kitsahawong, I am a full-time pediatric dentist and Associate Professor in the Faculty of Dentistry, Khon Kaen University. I was one of the long-term (PhD) trainees in the Fogarty International Center Training Program in Clinical, Public Health and Behavioral Oral Health Research for Thailand under the collaboration between KKU and the University of Washington (UW). Through the generous support from NIH, I received the opportunity to attend the 2010 UW Summer Institute and subsequently enrolled in several epidemiology and biostatistics courses offered at the UW School of Dentistry during my first year in PhD in Oral Science program at KKU.
Hi, my name is Kemporn “Pom” Kitsahawong, I am a full-time pediatric dentist and Associate Professor in the Faculty of Dentistry, Khon Kaen University. I was one of the long-term (PhD) trainees in the Fogarty International Center Training Program in Clinical, Public Health and Behavioral Oral Health Research for Thailand under the collaboration between KKU and the University of Washington (UW). Through the generous support from NIH, I received the opportunity to attend the 2010 UW Summer Institute and subsequently enrolled in several epidemiology and biostatistics courses offered at the UW School of Dentistry during my first year in PhD in Oral Science program at KKU.
I am deeply indebted to Professor Timothy A. DeRouen, Dean Waranuch Pitiphat, Dr. Ana Lucia Seminario and Dr. Christy McKinney who had tirelessly advised me to expand my perspectives and to seek opportunities to do research during my time at Seattle. These experiences increased my knowledge in research, especially in the clinical trials. In addition, my experiences in working with professionals at the IRB for human research ethics had tremendously improved the understanding of this issue among the participants and conducting good clinical research later on.
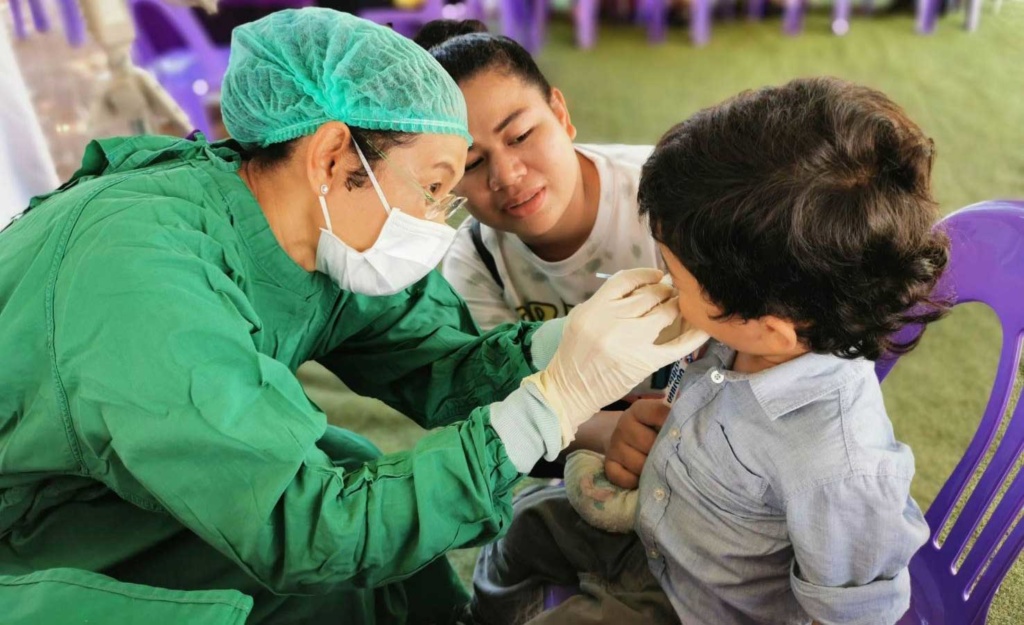 Over the past 10 years after my training with the UW team, I have been assisting Dean Pitiphat in expanding the knowledge and expertise in clinical oral health research to LMIC’s in Asia. The International Workshops on “Clinical Research Methods in Oral Health” jointly organized by University of Washington, Thammasat University and Khon Kaen University was conducted every 2 years. In the recent workshops, I served as a mentor facilitating the trainees from the leading institutes in Southeast Asia countries on developing a research proposal. This was a great opportunity to be able to share the experience with several international participants and to build partnerships that have mutual benefits in this region. Regarding research support, I have received consecutive grants from KKU Research Unit, KKU Faculty of Dentistry and the Office of National Higher Education Science Research and Innovation Policy Council (NXPO). These allow my team to carry on our research and recruit additional junior clinicians into the team.
Over the past 10 years after my training with the UW team, I have been assisting Dean Pitiphat in expanding the knowledge and expertise in clinical oral health research to LMIC’s in Asia. The International Workshops on “Clinical Research Methods in Oral Health” jointly organized by University of Washington, Thammasat University and Khon Kaen University was conducted every 2 years. In the recent workshops, I served as a mentor facilitating the trainees from the leading institutes in Southeast Asia countries on developing a research proposal. This was a great opportunity to be able to share the experience with several international participants and to build partnerships that have mutual benefits in this region. Regarding research support, I have received consecutive grants from KKU Research Unit, KKU Faculty of Dentistry and the Office of National Higher Education Science Research and Innovation Policy Council (NXPO). These allow my team to carry on our research and recruit additional junior clinicians into the team.
Currently, I have been supervising research projects, both clinical and laboratory bases. I am mentoring master and PhD students to develop the skills required for conducting research in oral health. I have been working in collaboration with the KKU Faculty of Pharmaceutical Sciences to develop innovative treatment for pediatric patients. As part of the KKU medical hub, I have expanded my expertise in taking care of young patients who had medically compromised conditions and also those with special needs. Our dental school plays a major role in the KKU Cleft Center, which delivers multidisciplinary treatment for individuals with oro-facial clefts and craniofacial anomalies. This center has built upon the efforts of many medical and dental specialists, including pediatric dentists who provide oral health care and interceptive orthodontic treatment as part of the holistic protocol. These has given me the experiences in participating in such a competent network.
I believe that my expertise gained during these valuable years have armed me with the necessity competency to participate and lead the projects, particularly on the aspect of clinical research and oral health in children.


 Hi, my name is Janella Bermúdez and I’m currently a fourth-year dental student at the University of Washington. I am one of eight students selected to be in the Regional Initiatives in Dental Education (RIDE) Program, an educational track of the UW. Through community-based experiences, RIDE develops socially responsible dentists who foster a commitment to improving the oral health of vulnerable communities.
Hi, my name is Janella Bermúdez and I’m currently a fourth-year dental student at the University of Washington. I am one of eight students selected to be in the Regional Initiatives in Dental Education (RIDE) Program, an educational track of the UW. Through community-based experiences, RIDE develops socially responsible dentists who foster a commitment to improving the oral health of vulnerable communities. Joining the DeRouen Center
Joining the DeRouen Center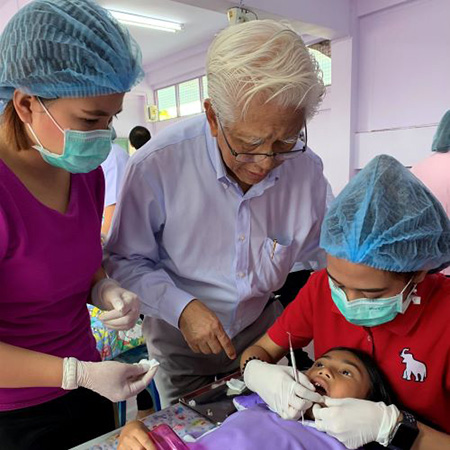 In the past decade, one of the activities of the WHO is to provide consultants to developing countries worldwide. I had the privilege to be short-term consultant for oral health in a few countries such as Dental education and dental public health in Laos PDR, and Myanmar; De-fluoridation to prevent fluorosis in Tanzania, India, and Sri Lanka; Atraumatic Restorative Treatment (ART) for appropriate dental restorations in Bhutan, Indonesia, and Syria. It was necessary to study the local health and oral health system and situation in advance, as well as seek the advice of local authorities during the visit. First-hand information about the people through direct dialogue was key input for the WHO consultants to develop a practical oral health plan with appropriate technology. My latest activities with the WHO was involvement in the Myanmar First National Oral Health Survey in 2016, followed by using collected data for planning the National Oral Health Strategy in 2018. Then in 2019, the Ministry of Health and Sport organized the WHO Regional side-meeting with the Asian Chief Dental Officers Meeting (ACDOM) in Mandalay, Myanmar.
In the past decade, one of the activities of the WHO is to provide consultants to developing countries worldwide. I had the privilege to be short-term consultant for oral health in a few countries such as Dental education and dental public health in Laos PDR, and Myanmar; De-fluoridation to prevent fluorosis in Tanzania, India, and Sri Lanka; Atraumatic Restorative Treatment (ART) for appropriate dental restorations in Bhutan, Indonesia, and Syria. It was necessary to study the local health and oral health system and situation in advance, as well as seek the advice of local authorities during the visit. First-hand information about the people through direct dialogue was key input for the WHO consultants to develop a practical oral health plan with appropriate technology. My latest activities with the WHO was involvement in the Myanmar First National Oral Health Survey in 2016, followed by using collected data for planning the National Oral Health Strategy in 2018. Then in 2019, the Ministry of Health and Sport organized the WHO Regional side-meeting with the Asian Chief Dental Officers Meeting (ACDOM) in Mandalay, Myanmar. The first step in my Fogarty journey was a one-week long orientation at the NIH Headquarters in Bethesda, MD. The first two days of orientation involved going through an intensive Methodology workshop, and trainees can choose between quantitative or qualitative methodology approaches, dependent on the nature of their project. In these workshops, you get a crash course in data collection, management, and analysis that is pertinent to global health research. Every morning of orientation, there were breakfast networking sessions with directors of different NIH centers. I was one of the two people involved in the field of dentistry, and the first dental student to have ever received the award, which gave me the opportunity to have casual conversation with the director of the National Institute of Dental and Craniofacial Research (NIDCR), Martha J. Somerman, DDS, PhD. It was a rare opportunity to have a one-on-one conversation over breakfast with the director, an opportunity I know many dental researchers will never have. Further, this Fogarty orientation period provided us with more opportunities to interact with some other greats: Anthony Fauci, the immunologist and director of the National Institute of Allergy and Infectious Disease who made significant contributions to HIV/AIDS research and advocacy and is now leading the nation in the battle against COVID-19; Francis Collins, the director of the NIH who also led the Human Genome Project; and Roger Glass, the director of the John E. Fogarty International Center.
The first step in my Fogarty journey was a one-week long orientation at the NIH Headquarters in Bethesda, MD. The first two days of orientation involved going through an intensive Methodology workshop, and trainees can choose between quantitative or qualitative methodology approaches, dependent on the nature of their project. In these workshops, you get a crash course in data collection, management, and analysis that is pertinent to global health research. Every morning of orientation, there were breakfast networking sessions with directors of different NIH centers. I was one of the two people involved in the field of dentistry, and the first dental student to have ever received the award, which gave me the opportunity to have casual conversation with the director of the National Institute of Dental and Craniofacial Research (NIDCR), Martha J. Somerman, DDS, PhD. It was a rare opportunity to have a one-on-one conversation over breakfast with the director, an opportunity I know many dental researchers will never have. Further, this Fogarty orientation period provided us with more opportunities to interact with some other greats: Anthony Fauci, the immunologist and director of the National Institute of Allergy and Infectious Disease who made significant contributions to HIV/AIDS research and advocacy and is now leading the nation in the battle against COVID-19; Francis Collins, the director of the NIH who also led the Human Genome Project; and Roger Glass, the director of the John E. Fogarty International Center. Justin is a third-year dental student at the University of Washington. He graduated from Brigham Young University with a degree in Physiology and Developmental Biology and is passionate about the health-care field. Justin lived in São Paulo, Brazil for two years as a volunteer through church and loves to learn about cultures and people around the world. He enjoys playing and spending time with his daughters and watching sports with his wife.
Justin is a third-year dental student at the University of Washington. He graduated from Brigham Young University with a degree in Physiology and Developmental Biology and is passionate about the health-care field. Justin lived in São Paulo, Brazil for two years as a volunteer through church and loves to learn about cultures and people around the world. He enjoys playing and spending time with his daughters and watching sports with his wife. I chose to go into public health because it is an interesting and ever-evolving field. As the current COVID-19 pandemic shows, once basic public health breaks down, people cannot work, take care of their families, or interact with their communities in a normal way. Public health is the pulse of our society – without basic metrics of public health people are not able to pursue their daily lives.
I chose to go into public health because it is an interesting and ever-evolving field. As the current COVID-19 pandemic shows, once basic public health breaks down, people cannot work, take care of their families, or interact with their communities in a normal way. Public health is the pulse of our society – without basic metrics of public health people are not able to pursue their daily lives. Why I chose dentistry
Why I chose dentistry

